 Just in time for Field Day and pool openings, today we provide sunburn protection information.
Just in time for Field Day and pool openings, today we provide sunburn protection information.
Hot!
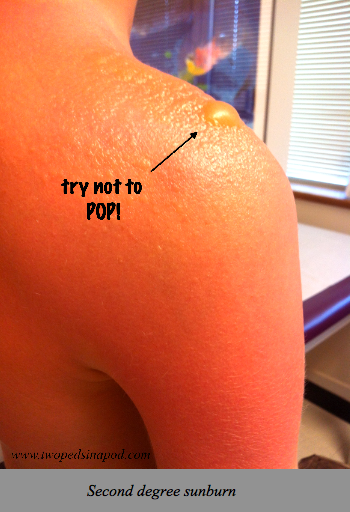
Pictured is a kid with a second degree burn. No, this burn wasn’t caused by hot water or by touching the stove, but by the sun. A sunburn is still a burn, even if it was caused by sunlight.
Treat sunburn the same as you would any burn:
- Apply a cool compress or soak in cool water.
- Do NOT break any blister that forms- the skin under the blister is clean and germ free. Once the blister breaks on its own, prevent infection by carefully trimming away the dead skin (this is not painful because dead skin has no working nerves) and clean with mild soap and water 2 times per day.
- You can apply antibiotic ointment to the raw skin twice daily for a week or two.
- Signs of infection include increased pain, pus, and increased redness around the burn site.
- A September 2010 Annals of Emergency Medicine review article found no best method for dressing a burn. In general, try to minimize pain and prevent skin from sticking to dressings by applying generous amounts of antibiotic ointment. Look for non adherent dressings in the store (e.g. Telfa™). The dressings look like big versions of the plastic covered pad in the middle of a Band aid®.
- At first, the new skin may be lighter or darker than the surrounding skin. You will not know what the scar ultimately will look like for 6-12 months.
- If the skin peels and becomes itchy after a few days, you can apply moisturizer and/or over-the-counter hydrocortisone cream to soothe the itch.
- Treat the initial pain with oral pain reliever such as acetaminophen or ibuprofen.
Preventing sunburn is much easier, more effective, and less painful than treating sunburn.
What is SPF? Which one should be applied to children?
- SPF stands for Sun Protection Factor. SPF gives you an idea of how long it may take you to burn. SPF of 15 means you will take 15 times longer to burn… if you would burn after one minute in the sun, that’s only 15 minutes of protection!
- The American Academy of Pediatrics recommends applying a minimum of SPF 15 to children, while the American Academy of Dermatology recommends a minimum of SPF 30. Dr. Lai and I both apply sunscreen with SPF 30 to our own kids.
- Apply all sunscreen liberally and often– at least every two hours. More important than the SPF is how often you reapply the sunscreen. All sunscreen will slide off of a sweaty, wet kid. Even if the label says “waterproof,” reapply after swimming.
- Watch out for sunlight reflecting off water as well as sunburning on cool days. One pediatrician mom I know was aghast at seeing signs posted at her kid’s school reminding parents to apply sun screen “because it will be in the 80’s” … kids burn on 60 degree days too. Lower temperatures do not necessarily mean less UV light.
Why does the bottle of sunscreen say to ask the doctor about applying sunscreen to babies under 6 months of age?
- Sunscreens were not safety-tested in babies younger than 6 months of age, so the old advice was not to use sunscreen under this age. The latest American Academy of Pediatrics recommendation is that it is more prudent to avoid sunburn in this young age group than to worry about possible problems from sunscreen. While shade and clothing are the best defenses against sun damage, you can also use sunscreen to exposed body areas.
- Clothing helps to block out sunlight. In general, tighter weaves protect better than loose weaves. However, a study from 2014 suggests regular clothing is as protective as expensive “sun-protective clothing.”
- Hats help prevent burns as well.
- Remember that babies burn more easily than older kids because their skin is thinner.
Which brand of sunscreen is best for babies and kids?
- For babies and kids, no one brand of sunscreen is better than another. Dr. Lai and I tell our patients to apply a “test patch” the size of a quarter to an arm or leg of your baby and wait a few hours. If no rash appears, then use the sunscreen on whatever body parts you can’t keep covered by clothing.
Remember when we used to call sunscreen lotion “suntan lotion,” and tolerating red, blistering shoulders was considered a small price to pay for a tan? Live and learn.
Julie Kardos, MD with Naline Lai, MD
rev ©2015 Two Peds in a Pod®



